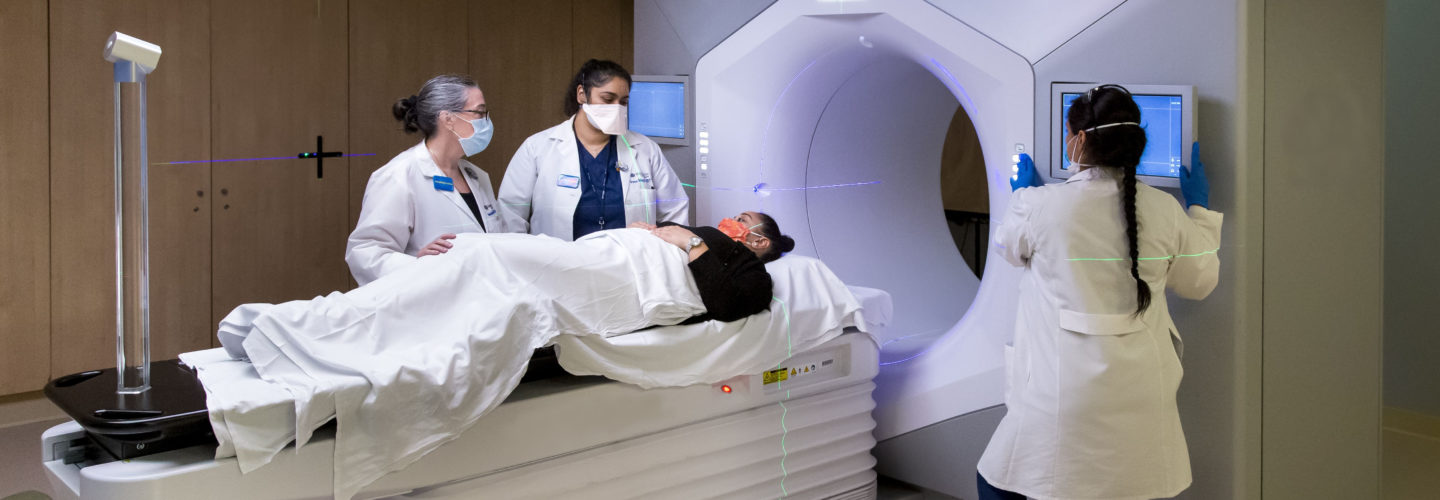
A wide range of technologies. Individualized treatment.
Radiation therapy (also called “radiotherapy” and frequently abbreviated as “RT”) is a type of cancer treatment that uses high doses of ionizing radiation to kill cancer cells and shrink tumors. It generally is delivered by a machine called a linear accelerator with high-energy X-rays, but electrons can also be used. It is estimated that 60% of all patients with cancer will require radiation therapy at some point in their treatment journey. The Radiation Oncology Department at Maimonides Cancer Center employs a wide range of modern technologies to deliver the radiation treatment best suited to each individual patient’s needs.
Your radiation oncologist will work with the rest of the radiation therapy team to determine which radiotherapy techniques are right for you, based on tumor type, location, and size. Then they will develop your treatment plan, oversee treatment, and monitor your progress.
External beam radiation therapy
External beam radiation therapy uses a beam or beams of radiation to treat tumors. It involves a series of daily outpatient treatments that may last for a few days or for several weeks. We offer the following types of external beam radiation therapy.
Adaptive radiation therapy (ART)
Used for certain types of tumors, ART leverages hyper-fast imaging and artificial intelligence (AI) to scan patients more often and adjust treatment plans in real time. This shortens treatment duration, increases precision, and boosts the efficacy of each dose of radiation while sparing healthy tissue and maintaining safety for patients.
Electron beam therapy
Electron beam therapy is a less penetrating radiation that spares underlying tissues. It is best for patients whose cancers are near their skin’s surface or for tumors in the skin.
Ethos linear accelerator (LINAC)
Ethos therapy delivers personalized cancer care quickly, safely, accurately, and comfortably. This advanced, state-of-the-art technology enables daily adjustments to radiotherapy treatment, thereby improving the targeting of tumors. Throughout treatment, changes in your anatomy may occur; tumors can shrink, and healthy tissues and organs can shift around the tumor’s location. Ethos therapy utilizes advanced technologies to detect these changes, enabling us to modify your treatment plan accordingly. The effectiveness of this highly personalized approach is based on the ability to use multiple images captured by your care team to tailor your treatment plan, minimizing the risk of cancer recurrence and the severity of treatment side effects.
Image-guided radiation therapy (IGRT)
IGRT uses imaging technologies, such as cone beam computed tomography, during treatment to more accurately and safely deliver radiation to cancer cells.
Intensity-modulated radiation therapy (IMRT)
IMRT further enhances radiation precision, often allowing the delivery of a higher and more effective dose, while limiting exposure of healthy tissues.
Stereotactic body radiotherapy (SBRT)
SBRT uses large doses of focused radiation delivered in just a few treatments to destroy certain types of tumors more precisely and quickly than other techniques.
Surface-guided radiation therapy (SGRT)
SGRT uses infrared technology to create a map of the body’s surface, which helps our team ensure that the patient is in the optimal position during treatment. If the patient moves, this system will turn off the treatment so radiation is only delivered to the targeted area. This can also be used to perform “gating” or “deep inspiration breath hold” where the treatment is only delivered during part of the breathing cycle to increase treatment precision.
Three-dimensional conformal radiation therapy (3D-CRT)
3D-CRT uses sophisticated computers and CT or MRI scans to create detailed, 3D representations of the tumor and surrounding organs. This allows your radiation oncologist to shape radiation beams to the size and shape of the tumor and direct them precisely, sparing healthy tissue.
Brachytherapy
Also called internal radiation, brachytherapy uses special applicators to permanently or temporarily implant a radioactive source inside or close to a tumor, allowing a large dose to target cancer cells with less exposure to healthy tissue. Brachytherapy may require anesthesia and/or brief hospitalization.
Isotope therapy
Isotope therapy involves the administration of radioactive substances, usually in liquid form through an IV, to deliver radiation to cancer cells while delivering minimal doses to surrounding healthy cells. Our radiation oncologists have extensive experience in the use of a variety of isotopes including their use for the treatment of metastatic prostate cancer.
Managing radiation side effects
Patients may experience side effects from radiation therapy which vary based on the type of tumor being treated, the course of RT, and an individual’s response to treatment. The most common side effect is fatigue, and other side effects are usually related to the area being treated. For example, irradiated skin may feel sunburnt, while radiation of the throat may cause soreness during swallowing. Your care team will discuss what side effects should be expected and how they should be managed.
Caring for yourself before, during, and after radiation therapy
When undergoing radiation therapy, it is important to:
- Eat a balanced, nutritious diet
- Get plenty of rest
- Seek emotional support
- Treat irradiated skin with extra care
- Avoid smoking, as it can interfere with radiation treatments
Call 718-765-2500 to make an appointment with an oncologist