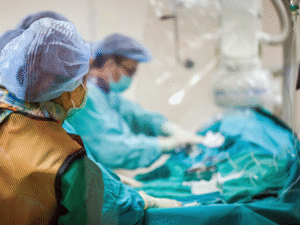
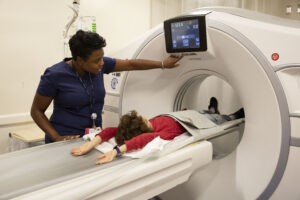
Maimonides Health’s Women’s Health Institute provides an individualized, patient-focused care partnership to women throughout every stage of life. For routine or specialty services, from adolescence to childbirth to menopause and beyond, Brooklyn patients can access the highest level of OB/GYN care close to home.
For patients with confirmed or unconfirmed gynecologic cancers and precancerous conditions, Maimonides offers exceptional diagnostic and therapeutic services, as well as preventive care through routine screenings and specialty services for patients at heightened risk.
“Our gynecologic oncology program is an essential part of the full-spectrum women’s health care we provide here at Maimonides,” said Scott Chudnoff, MD, Chair of Obstetrics and Gynecology. “Our approach centers around clinical excellence, patient comfort and experience, and enhancing quality of life for our patients facing these challenging conditions, as well as an emphasis on preventive care.”
Comprehensive, multidisciplinary reproductive cancer care
With the backing of the many specialties represented across the Women’s Health Institute and Maimonides’ renowned Cancer Center, expert clinical teams and dedicated support staff take a comprehensive approach to treating reproductive cancers.
The most common gynecologic cancers include:
- Uterine
- Cervical
- Vulvar
- Ovarian
- Vaginal
- Gestational trophoblastic disease (cancer of pregnancy-related tissue)
“In addition to invasive cancers, we also treat premalignant conditions in in the cervix, vagina, and uterus, undiagnosed pelvic masses, abnormal bleeding, and genetic mutations that can confer a higher risk of cancer,” says Manolis Tsatsas, MD, gynecologic oncologist at Maimonides.
The reproductive cancer care program at Maimonides encompasses the entire spectrum of care for cancer patients, including but not limited to:
- Medical oncology (chemotherapy)
- Radiation therapy
- Surgery, including minimally invasive techniques and robotic-assisted surgery
- Survivorship and long-term follow-up care
- Palliative care
- Hyperthermic intraperitoneal chemotherapy (HIPEC), to treat cancers that have spread to the lining of the abdominal cavity
Advanced surgical and medical therapies
Surgical care is a critical element of gynecologic oncology care. Maimonides surgeons perform advanced laparoscopic, robotic, hysteroscopic, abdominal, and vaginal surgery for complex, benign, and malignant gynecologic conditions.
“Our gynecologic oncology team possesses extensive experience in surgical therapies for cancer,” says Ioannis Alagkiozidis, MD, Director of Gynecologic Oncology at Maimonides. “That means that patients in Brooklyn benefit from high-level expertise in cancer treatment and prevention, and benefits like shorter recovery time, less pain and bleeding, and greater precision in procedures.”
Maimonides’ Robotic Surgery Program is the largest in Brooklyn, and host to gynecologic surgeons who perform more than 400 robotic procedures a year for both cancerous and noncancerous conditions. Albert Palileo, MD, gynecologic oncologist, and Justin To, MD, Associate Chair of Gynecology, join Dr. Alagkiozidis and Dr. Tsatsas in providing robotic and minimally invasive surgical therapies to reproductive cancer patients.
Maimonides gynecologic oncologists are well-versed in the most effective medical and radiation therapies to be utilizedindependently or in combination with surgical therapies, reinforced by the multidisciplinary expertise of clinicians at Maimonides Cancer Center, the borough’s only full-service cancer center.
Maimonides connects patients to national clinical trials through the National Cancer Institute and American Cancer Society via the Cancer Center, as well as to gynecologic oncology–specific clinical trials through NRG Oncology’s Gynecologic Cancer program. These clinical trial resources allow patients access to the most innovative new therapies during their treatment at Maimonides, improving individual and field-wide standards of care and quality of life during and after treatment.
Regional leadership in training and clinical practice
Maimonides’ Gynecologic Oncology Fellowship is a unique collaborative partnership between Maimonides Medical Center, SUNY Downstate, and NewYork Presbyterian–Methodist Hospital, in which fellows rotate between Maimonides and SUNY Downstate every three months during the two clinically focused years of training. During the third and final year of the fellowship, participants pursue research initiatives and complete a semester at SUNY’s School of Public Health, focusing on epidemiology and biostatistics.
This ACGME-accredited program prepares physicians to become expert specialists in treating ovarian, uterine, cervical, and vulvar malignancies. Fellows gain extensive clinical experience through direct patient care, surgical procedures, and multidisciplinary collaboration with medical oncologists, radiation oncologists, and pathologists.
“Our program is one of the country’s oldest gynecologic oncology fellowship programs, active for more than five decades,” says Dr. Alagkiozidis, who also serves as Fellowship Director. “Our fellows actively participate in the entire spectrum of care for our cancer patients, from surgical care to chemotherapy to palliative and survivorship care and everything in between. We aim to train gynecologic oncologists to excel not only in clinical practice, but also in research, academics, administration, leadership, and most importantly, expertise in patient care.”
Maimonides’ regional expertise and collaboration with other Brooklyn healthcare institutions also extends beyond the fellowship program. Starting in summer of 2025, Dr. Tsatsas and Dr. Palileo began an initiative to provide clinical support for gynecologic oncology services offered at NYC Health + Hospitals/South Brooklyn Health. Through this collaboration, patients benefit from greater access to the most cutting-edge care for reproductive cancers.
Addressing and managing precancerous conditions
In addition to treating confirmed malignancies, assessing and treating precancerous conditions is a critical element of Maimonides’ gynecologic oncology practice. Precancerous conditions can often be identified in routine gynecologic preventive care, offering a critical opportunity for specialized management to prevent cancer from occurring.
“With common precancerous conditions like cervical dysplasia and endometrial hyperplasia, many patients don’t experience any symptoms, so early identification through regular screening is essential,” says Dr. Tsatsas. “Once identified, our team can help patients explore options to decrease their cancer risk, like prophylactic surgery or ongoing observation.”
Genetic mutations also significantly influence gynecologic cancer risk. BRCA1 and BRCA2 mutations substantially increase the likelihood of ovarian and breast cancers. Women with known genetic predispositions require more aggressive monitoring and may also benefit from preventive measures like prophylactic surgery or enhanced surveillance protocols.
Partnering with patients and providers to assess risk factors and warning signs
Gynecologic cancers often show few to no clear signs before diagnosis. Aside from known malignancies and positive biopsy results, patients and providers alike should be aware of potential warning signs that merit biopsy testing and/or advanced referral to a gynecologic oncology specialist, including:
- Abnormal masses
- Cystic lesions
- Abnormal bleeding
- Precancerous conditions like cervical dysplasia and endometrial hyperplasia
- Genetic markers and family history
“About 20% of ovarian cancer incidences are thought to be genetically influenced,” says Dr. Tsatsas. “Providers can investigate whether their patients may be at heightened risk through direct testing, family history assessment, or genetic testing results of immediate family members. Diagnosing an abnormal mutation means that a patient is at increased risk of cancer, so at that point our multidisciplinary teams collaborate to make recommendations to abate that risk, including preventive surgery to remove affected tissue, depending on the mutation.”
Screening for cervical cancer
Regardless of genetic factors, all women should be screened for cervical cancer at appropriate intervals. Almost allcervical cancers are caused by sexually acquired infection from the human papillomavirus (HPV).
“Most women who acquire cervical cancer will do so in their reproductive years, so, the most common symptom, which is abnormal bleeding, may often be missed,” says Dr. Tsatsas.
The mainstay of diagnosing cervical cancer is through a screening test known as a Pap smear. All women should have routine Pap smear testing starting at the age of 21, repeating that test every two to three years up until age 30. After age 30, testing gets spaced out to every five years.
HPV testing has also emerged over the past decade, allowing clinicians to identify patients at the highest risk for cervical cancer before any abnormal screening findings can be identified.
“We’re fortunate to have reliable testing for HPV and cervical cancer, which makes a huge difference in treatment efficacy, survival rates, and preservation of organ function,” says Dr. Tsatsas. “For stage 1 cancer, the survival rate is more than 90%, compared to less than 20% for those diagnosed at stage 4.”
“Every year, our field is advancing. We’re saving more lives from reproductive cancers, and we can even prevent some cases before they even occur,” says Dr. Alagkiozidis. “Our team is proud to bring this world-class level of care and expertise to our patients and to be a partner to primary care and women’s health physicians across the borough.”
Learn more about gynecology and women’s health services at Maimonides. To schedule an appointment or refer a patient, call 718-283-9044.